My name is Rhonda, and this is the story (so far) of my wonky heart valve.
I found out that I had a problem with my mitral valve—one of four valves and that open and close to let blood flow through the heart—when I was in my early 20s. I wasn’t told much about it, other than that I probably had strep as a kid and needed to start taking antibiotics before any dentist visits. A decade later, I found myself needing a valvuloplasty (involving the insertion of a balloon to widen the narrowing valve opening and done under mild sedation). I was told that would last 15-20 years, a length of time that seemed unimaginable in my early 30s.
Fortunately for me, I felt very healthy from that point onward—until I noticed, at a party just before Christmas 2014, that I couldn’t dance. I just didn’t have the breath for it. I recognized the feeling immediately, but that was the only symptom, so I figured I had time enough to get this sorted.

Wapcaplet, CC BY-SA 3.0, via Wikimedia Commons
In 2015, my physician referred me to a cardiologist. I had been living in Toronto when I had my valvuloplasty, but here in CBRM I was starting over. I received a call to see a cardiologist in 2018. I was more than ready to action this now.
The next two years were filled with lots of tests to monitor the state of that mitral valve: stress tests, echocardiograms, hell, I can probably do an EKG myself now. I had a cardiac catheterization (dye test) in Halifax in June 2019. The valve was tight, but I was still on my feet. I knew I needed a new valve, but I had one stipulation: NO open-heart surgery.
During these years, I had done a lot of research about replacement valves. Who was doing what where, improvements in procedures and patient outcomes. Not that I was any expert, but I was getting an idea of what I wanted my outcome to look like.
I decided that I wanted to go to the Heart Centre at Saint John Regional Hospital in New Brunswick.
In late 2019, I met with a surgeon from Halifax, explained my journey to that point and told him of my desire (no offense intended) to go to Saint John for my surgery. He referred me to a colleague in Saint John who was performing minimally invasive mitral valve replacements, among other cardiac surgeries and five weeks later, in January 2020, my husband and I were on our way to Saint John for my consultation.
Finally!
In Saint John the surgeon listened to me, explained how the operation was performed, how tiny the new valve is before it’s “’installed” and how satisfied patients were with the outcome. He just needed the records from my 2019 dye test, he said, and the surgery should probably be done before summer.
But we all know what happened in March 2020: everyone’s plans were gone with the wind.
In July 2021, I got a call from Saint John Regional. They needed me there August 6, they wanted to do a second dye test. Off we went to New Brunswick and I had the test again. Afterwards, my surgeon came to see me and told me the valve was in a severe state. (At this point, I was unaware that I was on a surgical list. I didn’t know about it until three months later, when I was told I was #41 but with COVID doing its worst, no one could estimate how long it would take me to climb the list.)
OK, so at this point I should say I had never had “real” surgery – meaning an operation where I was put to sleep using general anesthetic. Things I was worried about: what if I wake up during the operation? What if I wake up afterwards and I have a ventilator, will I panic? Someone told me that anesthesia makes you vomit when you wake up. Someone else told me that my mouth would be very dry when I woke but I wouldn’t be allowed to drink water. Were these things true? (As it turned out, none of this happened.)
When I was told in December 2022 that my surgery was happening in January 2023, I was relieved, excited and completely ignorant of what lay before me.
This was lifesaving surgery for me. By December 2022 I was really run down. When I woke in the morning, I had six hours to do whatever I was doing that day. Laundry? Dishes? Maybe a dash out to my place of work to do a couple hours of filing and organizing receipts or some invoice processing at home? COVID was (and is) a mortal enemy, so I was not doing anything much outside the house. I didn’t have the breath to walk more than 20 feet. I had to plan and organize my day to ensure I climbed the stairs as few times as possible. Usually by 2 PM I was in bed with a book, and that was it for the day.
But I was full of hope and plans for the future. I wasn’t giving up. No way.
The week of my surgery, we left for New Brunswick at 5:00 AM on a Monday. It rained until we reached the Cobequid Pass then turned to freezing rain the rest of the way to Saint John. We arrived with time to spare and were shown to my room where I was descended upon by nurses, pharmacists, dietitians, people with paperwork and my surgeon. Still shaking because of the stress of the drive, I burst into tears and was given some space while my surgeon spoke to me. When he left, two nurses approached. I had no IV pole to drag around but I did have an IV taped to my left arm at my elbow. I got a chest x-ray and a CT scan. My husband helped me get into my pajamas but he had to leave before it got dark to find the place where he would be staying.
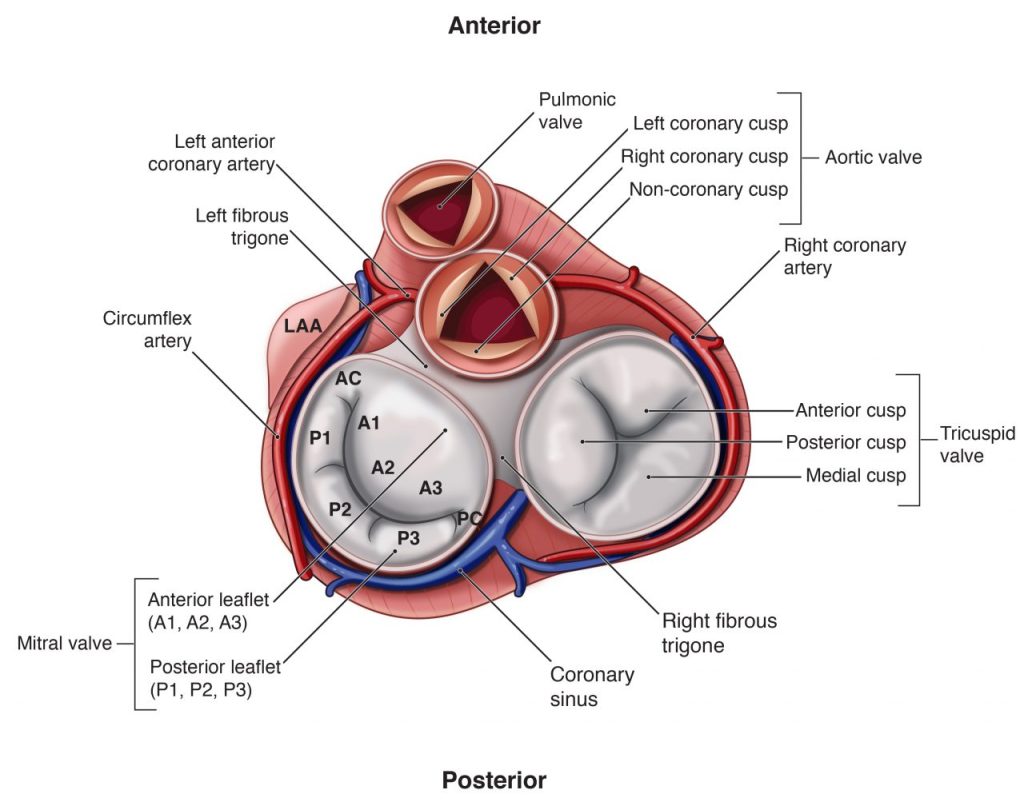
Mitral valve. (Source: Echoboards Academy)
The following day, Tuesday, was much the same with people coming and going. Wednesday’s highlight was my first pre-surgery scrub down. I prepared for this by having my hairdresser cut my hair into a pixie. I was given some disinfecting soap to methodically scrub myself head to toe. A few hours later, I was given an Ativan and I don’t remember anything until Friday.
My surgery was scheduled for Thursday at 8:00 AM. According to my husband, he arrived at the hospital at 6:30 AM. I may have a faint memory of this, but I’m not sure. I had to scrub myself again in the shower, and I was given some medication that made me very “high.” Then I was carted off to surgery.
I had been given a booklet by the hospital back in 2021. It stated that minimally invasive mitral valve surgery took three hours—mine took six. My husband was frantic, and it was probably at this point that everything we thought we knew about what was to come went out the window.
Of course, we were told I’d have surgery, would be moved to ICU to stabilize, then moved again to the “step-down” room, and then finally back onto the floor. But we had no firsthand knowledge of “heart surgery,” anyone we knew of who had had heart surgery lived somewhere else. It was major surgery, of course, but about the actual day-to-day of the first-few-days and recovery we knew nothing.
The surgical team was top drawer, and I was completely confident of a smooth procedure. I’m not sure my husband should have seen me in ICU, I hadn’t prepared him for that. That freaked him out.
I do remember being woken up in ICU by my surgeon on Friday. He must have said something along the lines of, “Hello, it’s Friday!” because I imagined I asked him what day it was, but of course, I probably couldn’t speak. I fell back asleep, and my next memory was of being in the step-down room. There were four patients in that room, but in my chemically-altered state, it felt like I had a crowd around me. I wasn’t aware of any discomfort other than thirst. Morphine shots were getting me through, and the nurses were giving me sips of water.
That weekend in Saint John there was a major snowstorm, and patients who were scheduled to leave were delayed, which meant my stay in the step-down room was prolonged. It was odd in there with constant machine alerts as background noise. I won’t really go into it, but during this time staff had to remove tubes left over from ICU (not pleasant). I didn’t mind getting out of bed to sit in my chair. The step-down room seemed to be heavy on tall, male nurses and they easily maneuvered me out of the bed, I felt no discomfort at all. Plus, they gave me a small, firm pillow to clutch when I sneezed or coughed.
After two days, they stopped administering morphine. They gave me a hydromorphone pill, and my stomach did not like that at all. They had also been giving me two Tylenol every four hours and from that point on, it was just Tylenol, and I was fine.
What I really struggled with in hospital after my surgery was twofold: I had “pacemaker” wires inserted under my skin around my right shoulder blade that were covered with cotton wool, so I had a lump on my back that prevented me from lying down comfortably; and I had lost my sense of taste, in that everything I ate tasted like mud, so I wasn’t really eating. I was tired and hungry.
I was brought back onto the floor Tuesday morning. No sleep that night. They removed the wires shortly before we left for home on Wednesday. Ugh. I’d have to wait the better part of two weeks to taste food properly again.
It wasn’t easy being home at first. I was afraid of my incision, would I be able to use my arm normally again, how long would I feel like this? It did turn out that a new blood pressure pill was not agreeing with me, and my cardiologist took me off it.
The sun came out.
I’m not quite healed on the outside, between the incision and my skin (the tape they use in hospital is brutal) but I’m noticing more healing on the inside, prickles, and sore spots, but this is normal recuperation. Recovery is definitely not 2-3 weeks, more like 6-8, I’m discovering. But I’m almost there, and excited for a new healthy me!
Rhonda MacDougall-Gale is from Sydney Mines and, by way of Halifax and Toronto, now lives in South Bar with her husband.








